Type 5 diabetes, previously known as malnutrition-related diabetes mellitus (MRDM), is a distinct form of diabetes linked to chronic undernutrition and health disparities. The condition primarily affects people in low- and middle-income countries (LMICs), especially in South-East Asia and sub-Saharan Africa.
MRDM was formally classified as type 5 diabetes at an international meeting of experts convened in January 2025. The new classification was endorsed by the International Diabetes Federation (IDF) at the World Diabetes Congress 2025 in Bangkok, Thailand. The condition is now acknowledged as the fifth classification of diabetes, alongside types 1, 2, 3c and gestational diabetes. This recognition marks a significant step towards addressing a long-overlooked condition and advancing health equity in diabetes care for the millions affected globally. The classification also helps improve understanding of metabolic health in young adults living in under-resourced conditions.
Causes
Type 5 diabetes results from prolonged undernutrition, particularly during early childhood and adolescence. Poor maternal nutrition, frequent infections and chronic food insecurity can impair the development of the pancreas. This reduces its ability to produce insulin. Damage to the pancreas is not the result of autoimmune reactions, as in type 1 diabetes, or insulin resistance, as in type 2 diabetes. Instead, it is a non-autoimmune diabetes type, caused by an inability of the pancreas to produce enough insulin due to underdeveloped pancreatic tissue.
The condition highlights the impact of poverty on health outcomes, particularly in communities where people face lifelong nutritional deficits. Refugees and migrants from resource-poor settings may also be at risk, even after resettling in high-income countries.
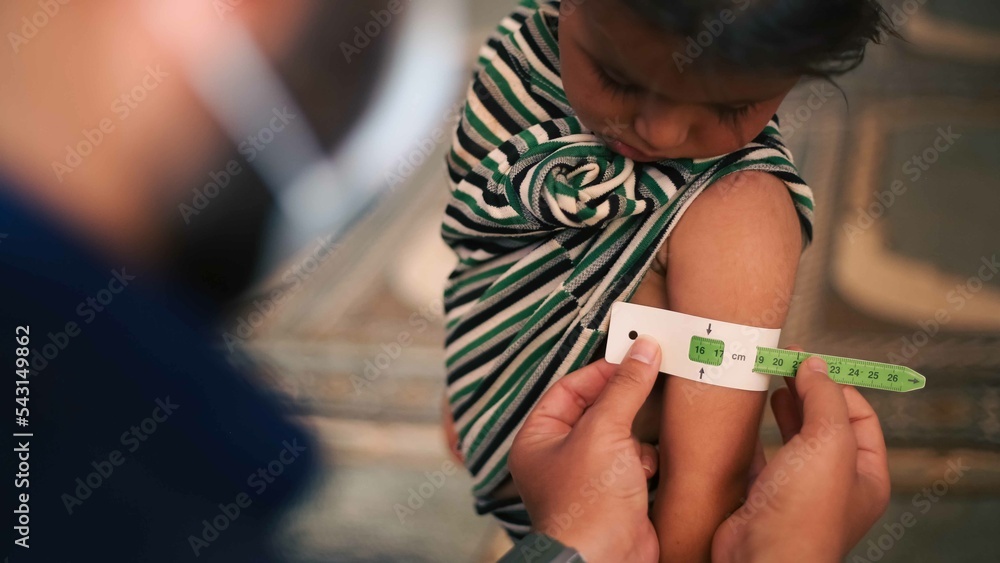
Symptoms
Type 5 diabetes typically appears in adolescents and young adults and may present symptoms similar to type 1 diabetes, such as:
- Weight loss
- Excessive thirst
- Frequent urination
- Fatigue
- Elevated glucose levels
However, people with type 5 diabetes often have a body mass index (BMI) below 19 kg/m² and do not show signs of autoimmune β-cell destruction, which distinguishes it from type 1 diabetes.
Diagnosis
Until recently, there were no standard diagnostic criteria for type 5 diabetes. As a result, many people were incorrectly diagnosed with type 1 or type 2 diabetes and received treatments that did not meet their specific needs. This led to poor outcomes and further entrenched inequalities in care.
Treatment
Managing diabetes in resource-poor settings requires context-specific strategies. For type 5 diabetes, treatment must focus not only on glucose control but also on addressing nutritional deficits. Management may include:
- Nutritional support to correct long-term undernutrition.
- Oral diabetes medications to stimulate insulin secretion.
- Low-dose insulin therapy, where appropriate.
Standard treatments for type 1 or type 2 diabetes may not be effective for people with type 5 diabetes. As the root cause is insulin deficiency linked to undernutrition, a tailored treatment plan is essential. Without proper care, there is an increased risk of complications such as nerve damage, kidney disease and vision problems. Life expectancy may be significantly reduced if the condition is not diagnosed and treated accurately.
Prevention
Preventing type 5 diabetes involves addressing the root causes of chronic undernutrition and health inequality. Key areas of prevention include:
- Improving maternal nutrition and reducing diabetes risk in early life.
- Strengthening child nutrition programmes.
- Ensuring food security in vulnerable regions.
- Reducing poverty and infection risk.
Early nutritional interventions and health policies that strengthen primary care access can reduce the incidence of type 5 diabetes and contribute to lowering the global diabetes burden.

Type 5 Diabetes Working Group
The International Diabetes Federation has established a Working Group to develop formal diagnostic criteria to help healthcare providers distinguish type 5 diabetes from other types and to support accurate and timely treatment.
Chaired by Dr Meredith Hawkins and co-Chaired by Dr Nihal Thomas, the Working Group will also create a global patient registry to gather data, and support research and design training modules for healthcare professionals, particularly in LMICs
These efforts aim to increase awareness, reduce misdiagnosis and promote equity in diabetes care.