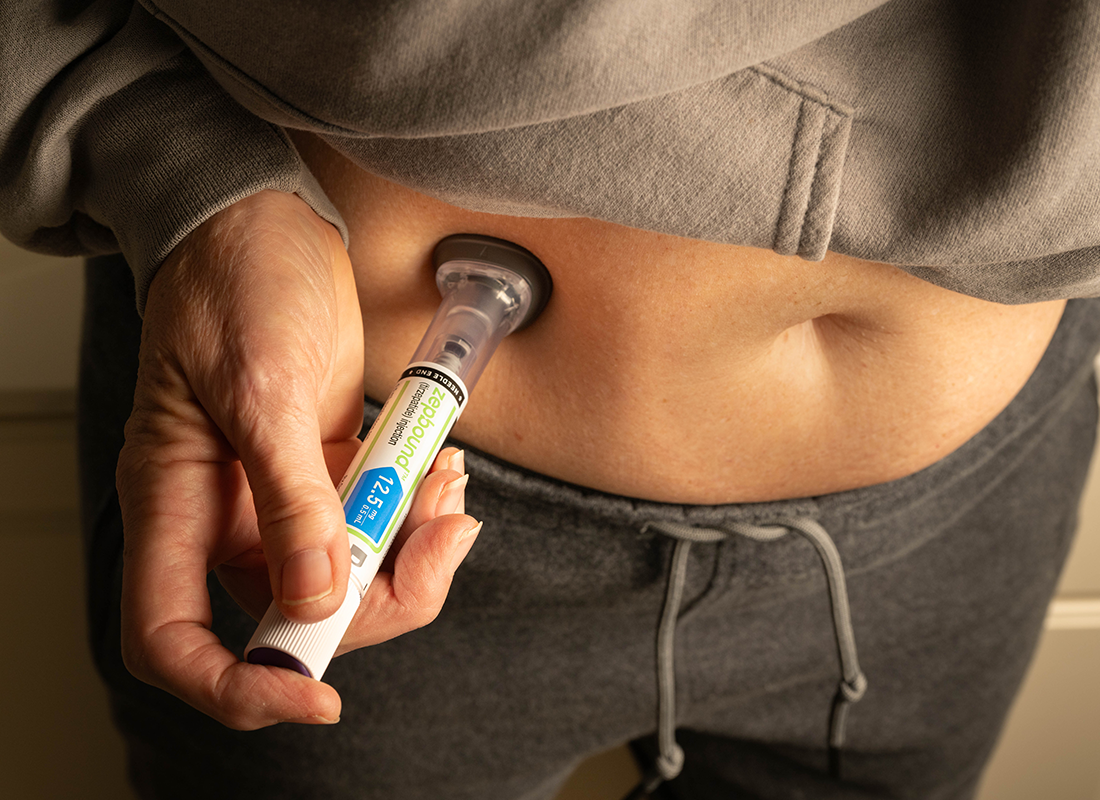
Non-insulin injectable medicines (GLP-1 & GIP) are treatments that help people living with diabetes manage blood glucose levels. They are taken as injections under the skin. Unlike insulin therapy, they do not replace insulin. Instead, they support the body’s natural hormone systems that help regulate blood glucose.
Two main groups of non-insulin injectable medicines are commonly used to manage blood glucose are glucagon-like peptide-1 receptor agonists (GLP-1 receptor agonists) and dual glucose-dependent insulinotropic polypeptide (GIP).
These medicines act on hormones in the digestive system known as incretins. Incretin hormones are released after eating and help control blood glucose levels. They stimulate the pancreas to release insulin when blood glucose rises and reduce the release of glucagon, a hormone that increases blood glucose. They also slow stomach emptying and may reduce appetite.
This combined effect can help improve blood glucose management, particularly after meals. Some GLP-1 medicines have also been shown to reduce the risk of certain cardiovascular complications in people living with type 2 diabetes.
Why are GLP-1 and GIP medicines used?
Type 2 diabetes develops when the body does not use insulin effectively. This is known as insulin resistance. Insulin helps move glucose from the bloodstream into the body’s cells so it can be used for energy. When insulin does not work properly, glucose builds up in the blood.
Over time, the pancreas may also produce less insulin. In addition, the body’s incretin hormone response may become weaker. Normally, these hormones help regulate blood glucose after meals by increasing insulin release and reducing glucagon production.
GLP-1 and GIP medicines strengthen this natural system. They help the body respond more effectively to rising glucose after eating and reduce the amount of glucose released by the liver. Together, these actions support more stable blood glucose levels throughout the day and may improve overall diabetes management.
Who benefits from GLP-1 and GIP medicines?
Non-insulin injectable medicines are usually prescribed for people living with type 2 diabetes when blood glucose levels remain above target despite lifestyle changes and treatment with oral medicines. Because people with type 1 diabetes do not produce insulin, non-insulin injectable medicines cannot replace insulin therapy, but can be used as an additional treatment.
Starting treatment
Treatment with GLP-1 or GIP medicines usually begins after discussion with a healthcare professional. The healthcare team reviews blood glucose measurements, HbA1c results, current medicines, body weight and overall health. This helps determine whether these medicines are appropriate.
Most medicines in this group are supplied in pre-filled injection pens designed for use at home. Healthcare professionals provide instructions on how to use the device and how often to take injections. Depending on the medicine, injections may be taken once daily or once weekly.
Follow-up appointments are usually recommended after treatment begins. These visits allow healthcare professionals to review blood glucose levels, monitor progress and adjust treatment if needed.
Treatment and management
Non-insulin injectable medicines are usually part of a broader plan for managing type 2 diabetes. Medicine works best when combined with a healthy lifestyle.
This includes balanced nutrition, regular physical activity and monitoring blood glucose levels as recommended by a healthcare professional. Together, these steps help improve glucose management and support overall health.
Some people may experience side effects when starting treatment. The most common effects involve the digestive system and may include nausea, vomiting or stomach discomfort. These symptoms are often mild and usually improve as the body adapts to treatment.
Healthcare professionals may begin treatment with a lower dose and increase it gradually to help reduce side effects.
Living with GLP-1 or GIP treatment
For many people living with type 2 diabetes, non-insulin injectable medicines can become part of daily diabetes management. These treatments may help improve blood glucose control and, for some people, support weight management.
Although injections may feel unfamiliar at first, most injection devices are designed for easy use. With guidance from healthcare professionals, many people quickly become comfortable using them.
Living well with diabetes also involves regular health checks, monitoring blood glucose levels and maintaining a healthy lifestyle. Support from healthcare professionals, family members and community services can help people manage diabetes more effectively.
When to speak with a healthcare professional
People living with diabetes should speak with a healthcare professional if blood glucose levels remain above the recommended range despite current treatment. Discussion may also be helpful if there are concerns about weight management, side effects from medicines or questions about treatment options.
Healthcare professionals can review the current management plan and discuss whether medicines such as GLP-1 or GIP receptor agonists may be appropriate. Treatment decisions should always be made as part of a personalised care plan developed with a qualified healthcare professional.